Pediatric
- Pediatric Intro
- Exam Protocols
- Image Gallery
- Guidelines
- Bibliography
Three routes of US contrast agent administration have been described in children: intravenous (IV), intracavitary and oral.
- IV administration is typically used for characterization and detection of solid organ pathology, analogous to established IV uses in adults [6].
- Intracavitary contrast-enhanced US utilizes catheterization and includes intravesical administration for diagnosis of vesicoureteric reflux (VUR) and contrast-enhanced genitography for eval¬uation of ambiguous genitalia and cloacal malformations, both pediatric-specific indications [5, 8, 9, 14].
- Oral US contrast agent administration has only been described in one study involving the diagnosis of gastroesophageal reflux [15]. The procedures, uses and safety of IV and intravesical contrast-enhanced US in children are described below.
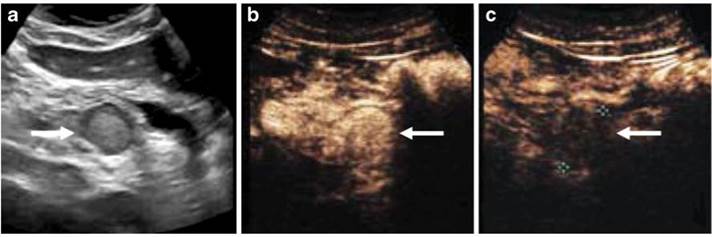
Pancreatic Neuroendocrine Tumor
Clinical example of contrast-enhanced US in a 14-year-old boy who collapsed playing rugby.
Prof. Christoph F. Dietrich, Department Allgemeine Innere Medizin (DAIM), Kliniken
Hirslanden Beau Site, Salem und Permanence, Bern, Switzerland
The European Federation of Societies of Ultrasound in Medicine and Biology (EFSUMB) first incorporated pediatric CEUS in its 2008 updated clinical practice guidelines and recommendations for CEUS:
EFSUMB’s current guidelines also address pediatric CEUS:
The European Society of Paediatric Radiology (ESPR) Uroradiology Task Force and the European Society of Urogenital Radiology (ESUR) Paediatric Working Group issued recommendations for pediatric CEUS imaging, primarily for intravesical administration, in 2008 and 2012:
1. Larson DB, Johnson LW, Schnell BM et al (2011) Rising use of CT in child visits to the emergency department in the United States, 1995–2008. Radiology 259:793–801
2. Pearce MS, Salotti JA, Little MP et al (2012) Radiation exposure from CT scans in childhood and subsequent risk of leukemia and brain tumors: a retrospective cohort study. Lancet 380:499–505
3. Brenner D, Elliston C, Hall E et al (2001) Estimated risks of radiation-induced fatal cancer from pediatric CT. AJR Am J Roentgenol 176:289–296
4. Goske MJ, Applegate KE, Boylan J et al (2008) Image Gently®: a national education and communication campaign in radiology using the science of social marketing. J Am Coll Radiol 5:1200–1205
5. Darge K (2010) Voiding urosonography with US contrast agent for the diagnosis of vesicoureteric reflux in children: an update. Pediatr Radiol 40:956–962
6. Piskunowicz M, Kosiak W, Batko T (2012) Intravenous application of second-generation ultrasound contrast agents in children: a review of the literature. Ultraschall Med 33:135–140
7. Papadopoulou F, Ntoulia A, Siomou E et al (2011) Safety of intravesical use of a second generation US contrast agent in children for vesicoureteric reflux detection. ECR Book of Abstracts, Insights Imaging 3:SS 1612, B-736
8. Darge K (2008) Voiding urosonography with ultrasound contrast agents for the diagnosis of vesicoureteric reflux in children. I. Procedure. Pediatr Radiol 38:40–53
9. Darge K (2008) Voiding urosonography with US contrast agents for the diagnosis of vesicoureteric reflux in children. II. Comparison with radiological examinations. Pediatr Radiol 38:54–63
10. Claudon M, Cosgrove D, Albrecht T et al (2008) Guidelines and good clinical practice recommendations for contrast enhanced ultrasound (CEUS) – update 2008. Ultraschall Med 29:28–44
11. Piscaglia F, Nolsøe C, Dietrich CF et al (2012) The EFSUMB guidelines and recommendations on the clinical practice of contrast enhanced ultrasound (CEUS): update 2011 on non-hepatic applications. Ultraschall Med 33:33–59
12. Riccabona M, Avni FE, Blickman JG et al (2008) Imaging recommendations in paediatric uroradiology: minutes of the ESPR workgroup session on urinary tract infection, fetal hydronephrosis, urinary tract ultrasonography and voiding cystourethrography, Barcelona, Spain, June 2007. Pediatr Radiol 38:138–145
13. Riccabona M, Avni FE, Damasio MB et al (2012) ESPR Uroradiology Task Force and ESUR Paediatric Working Group – Imaging recommendations in paediatric uroradiology, part V: childhood cystic kidney disease, childhood renal transplantation and contrast-enhanced ultrasonography in children. Pediatr Radiol 42:1275–1283
14. Kopac M, Riccabona M, Haim M (2009) Contrast-enhanced voiding urosonography and genitography in a baby with ambiguous genitalia and urogenital sinus. Ultraschall Med 30:299–300
15. Farina R, Pennisi F, La Rosa M et al (2008) Contrast-enhanced colour-Doppler sonography versus pH-metry in the diagnosis of gastrooesophageal reflux in children. Radiol Med 113:591–598
16. Darge K, Papadopoulou F, et al (2013) Safety of contrast-enhanced ultrasound in children for non-cardiac applications: a review by the Society for Pediatric Radiology (SPR) and the International Contrast Ultrasound Society (ICUS). Pediatr Radiol. 2013 Sep;43(9):1063-73.

