A 37-year-old male patient who was an intravenous drug abuser developed endocarditis (infection) of his heart valve, and surgery was urgently required to replace the valve because it was regurgitant (leaking). The patient continued to self-inject drugs and the new valve also became infected and started leaking badly.
The surgeons agreed to perform a second aortic valve replacement, but following continued drug use the newly replaced valve also became infected with large, mobile vegetations (infected masses) attached. One of the vegetations became detached and travelled down his right coronary artery causing an abscess cavity within the myocardium (heart muscle), and this can be seen on the echocardiogram in Figure 1, below.
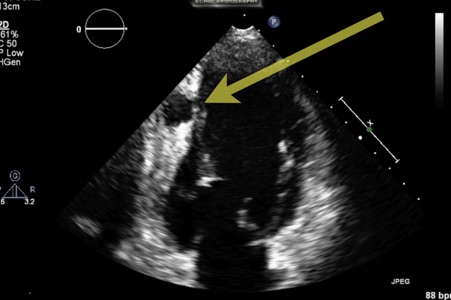
Despite the potential risk of rupture, the surgeons were reluctant to operate on this patient for a third time. They were, however, persuaded to change their minds and perform a life-saving operation after viewing the results of a Contrast Enhanced Ultrasound (CEUS) study that provided vital anatomical information about the abscess cavity.
Figure 2 shows two (apical 4 chamber & parasternal short axis) contrast enhanced views which demonstrate clear communication between the left ventricular cavity and the abscess cavity (arrowed). The contrast images also demonstrated that the abscess cavity was very pulsatile with a very thin tissue boundary between the abscess and the right ventricle.
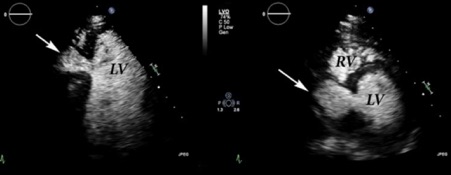
A contrast enhanced 3D scan was also performed (Figure 3 and Figure 4) and this also clearly demonstrated the pulsatile nature of the abscess (arrowed) and the danger of rupture into the right ventricle or into the pericardium (outside the heart) which would probably have been fatal.
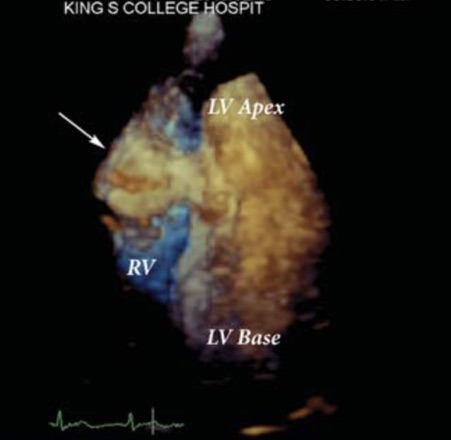
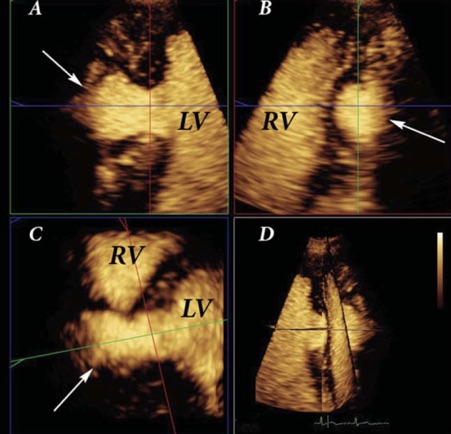
Based on these CEUS images, the cardiothoracic surgeons were convinced that they needed to re-operate on this young man to save his life. They successfully removed the abscess cavity and put in a tissue (pericardial) patch to repair the hole in the ventricular cavity.
Having been through three major cardiac operations as a direct result of his drug abuse, the patient finally agreed to receive therapy, has given up his drug habit, currently remains clean and is doing well!
Professor Mark J Monaghan PhD, FRCP (Hon), FESC, FACC is the Director of Non-Invasive Cardiology at King’s College Hospital, London, UK. He also is Secretary of the International Contrast Ultrasound Society.






